- In: operations
- 2 Comments
15.9.09
Meckel’s diverticulectomy 45M being operated for suspected appendicitis, actually had Meckel’s diverticulitis.
17.9.09
Burch colposuspension after TAH by dr Hans, colposuspension by me. Elderly obese lady. Used a mesh strip.
18.9.09
7.8.09
joined GMC Amritsar. surgery unit 3 (with dr gulati)
9.8.09
2 lap choles in patiala:
day case lap chole 10 at MS surgicare and
one more.
11.8.09
Assisted Dr Sukha Singh at TAH at his clinic (Amrit hospital) in Amritsar. Elderly lady with atrophic uterus. ? indicated or not?. Postop had severe abdominal pain and distension and vomiting, frightening the surgical team but eventually settled in 3 days.
13.8.09
MBBS final theory class in old LT in Amritsar medical college. CHPS.
17.8.09 monday
MBBS final theory class, continued with stomach – PU. Reached at 7.30 am from Patiala in time for the class.
20.8.09
last of these classes in amritsar, as JDA went on strike after this.
21.8.09
JDA on strike, junior doctors in Amritsar lathicharged by police in front of the OPD.
29.8.09
day case lap chole 11. previous ERCP and ES and stone extraction. Dr Kaler’s patient.
30.8.09 sunday
Went to chandigarh with mr Bhalla and saw the minister Tikshan Sood for transfer. He consented.
31.8.09
TLH , satisfactory.
8.9.09
To Amritsar and back, after having been relieved from there after transfe back to Patiala.
09.09.09
Joined at Patiala GMC again. good date to remember.
Also to remember was the first laparoscopic nephrectomy for non-functioning hydronephrosis (R). Very satisfactory. Specimen removed in a bag. Enjoyed.
11.9.09
A big ovarian cyst laparoscopically excised and removed in a bag.
13.9.08
two difficult cases:
a huge man 25 years old but very obese , more than 150 kg. Varicose veins ligated at saphenofemoral junction (Trendelenburg) plus multiple phlebecotomies.
Anderson Hynes pyeloplasty in a 7 years old male child. Stent not available. Drained.
22.6.09
Day case lap chole number 6: for the first time, port site (epigastric) bleeding caused a nuisance, controlled afterwards (after removing the gallbladder) by two sutures with port-closure needle.
23.6.09
Lap chole day case 7: Asha verma 55F, w/o popular school teacher here. short and wide CD, endlooped.
7.7.09
A disaster: trochar vascular injury during first trochar insertion for the camera in a case of diagnostic laparoscopy at Sehat, injuring the aortofemoral junction on the right side, leading to shock and a big haematoma, called in to repair, but unsuccessful. Patient succumbed. Sad day.
9.7.09
Emergency call for caesarean hysterectomy. Patient in shock. Saved after a quick hysterectomy at Babbar’s.
18.7.09
Repair of extensive vaginal lacerations at vaginal delivery conducted by a dai.
20.7.09
Accessory duct at day case 8 lap chole; doubly clipped and underrun too. OK in the end.
21.7.09
Bilateral TEP for recurrent bilateral inguinal herniae. 65M, related to the mess contractor of doctors’ hostel mess.
22.7.09
day case 9 lap chole, 40 F thin lady. Easy and nice postoperative period.
27.7.09
Failed retroperitoneal ureterolithotomy.
3.8.09
Relieved from GMC patiala for amritsar.
Joining govt service again, and some surgeries (including an adult intussuception and a hymenectomy).
Posted on: June 21, 2009
24.5.09
Acute gangrenous appendix removed laparoscopically urgently at 10 pm (c/o dr parminder from barnala). Young 12 male child.
27.5.09
A twisted ovarian cyst clinically and radiologically diagnosed, excised laparoscopically. 15 years old female with severe unremitting pain for 5 days (c/o milkman). However ovary was seen separate from the mass, and therefore it was surmised the mass was arising from the tube.
1.6.09
12 male child with a preoperative diagnosis of varicocele, causing pain. At inguinal exploration, had an indirect hernial sac which was the most likely cause of pain. Herniotomy and ligation of varicocele done.
4.6.09
Joined GMC patiala again as professor after the notice of premature retirement given in february was allowed to be withdrawn by the government.
5.6.09
Laparotomy for intestinal obstruction of some days standing. Remained admitted with medicine department with lots of investigations – including CT and BMFT but not operated. At operation, had intussusception – ileoileal. REEA done. A tumour within the lumen seen on cut section of the specimen.
7.6.09
day case lap chole 5. postop fever upto 101, settled in evening.
11.6.09
TLH satisfactory and complete.
12.6.09
TEP repair of left inguinal hernia. Very satisfactory and clean at last. 50 M with small direct hernia.
14.6.09
TLH satisfactory. Obese female 45 y o with posterior fundal fibroid.18.6.09
18.6.09
Hymenectomy for imperforate hymen. 17 F with big haematocolpos and haematometra.
21.6.09
a possible CBD injury:
an easy looking lap chole became difficult. 35F. while creating the posterior window and dividing the peritoneum posteriorly, bile leak noticed, presumable due to accessory duct. The patient was later found to have a RHD injury. Sad.
Converted lap chole and a failed TEP
Posted on: May 22, 2009
9.5.09
55 M (uncle of dr Pawan)- Thick walled gall bladder and unclear Calot’s triangle, eventually dissected out to find a wide thick cystic duct which was endlooped with vicryl and tied. While passing the ligature through the window, the instrument carrying the ligature had gone too far into the right loge of liver which bled, continuously and vigorously. Coagulating with diathermy spatula and passing a suture under having failed and with the patient getting into hypotension, converted into open surgery. However, the bleeding had stopped by then. Nonetheless, the injury was underrun. safe result eventually.
11.5.09
Difficult lap chole again. 45F with thickwalled empyema with big stone impacted at the neck. Fundus first dissection and neck of gall bladder closed from within.
13.5.09
Another difficult lap chole. 50 F. Big multiple stones, with one impacted in the neck, could not be disimpacted. The neck was opened up and all stones removed from within the gall bladder. Gall bladder cut up into 2 long ribbons to enable its removal without dilating the port.
15.5.09
2 lap appys at home.
A laparotomy for ileocaecal tuberculosis with intestinal obstruction. Had completed ATT. REEA done. Young (30) unmarried mentally disturbed patient (c/o Dr Phul Chandra).
17.5.09
day case lap chole 4
19.5.09
Vault prolapse following abdominal hysterectomy 12 years back. 60 F. Sacrocolpopexy with prolene 1.
20.5.09
Attempted TEP failed due to poor space maintenance. Converted to open.
21.5.09
Laparoscopic ovarian cystectomy left side. Medical student final year. Had pain lower abdomen, US showed a big ovarian cyst. Had ruptured leading to considerable blood loss.
6.5.09
Day case lap chole no 3. apparently OK when sent home. Next morning, reported severe pain abdomen, called back and hospitalised for an IV drip (RL). Clinically found nothing wrong, the abdomen soft and non-tender. Sent back home. ? tense and unnecessarily worrying patient.
7.5.09
Lap chole after pancreatitis. Saponifications seen very clearly, otherwise satisfactory procedure, no problems caused by the soaps.
9.5.09
Conversion in lap chole. 55M. Difficult procedure, short thick cystic duct, bigger than the clip, so end-looped with vicryl. While doing so, the Maryland carrying the ligature must have gone too far into the liver right lobe across the Calot’s triangle area. The injury continued to bleed rather excessively, pressure over it and surgicel over it not helping and patient going into hypotension. Therefore converted, but found the bleeding had stopped! Sutured the tear by an underrunning suture of 1 catgut.
Tryst with GSMC, and starting my own surgery, a hamartoma, a cystic hygroma, an intussusception etc
Posted on: May 7, 2009
20.2.09
Went to Gian Sagar Medical College, saw the chairman (mr Bhangoo) and vice-chairman (dr Sukhwinder singh), discussed with them about joining them and decided to do the same full time.
21.2.09
Gave joining report as Professor to dr Kamaljit singh CEO.
23.2.09
Went to GSMC, saw dr Sekhon (the principal) there, and changed the plan of working there to ‘retainer plan’. (retained for occasional visits).
27.2.09
Amputation b/k, diabetic 60M, infected and gangrenous leg. Wound kept open. Still got infected again later and the skin sloughed. Had to be refashioned after cutting further a bit of the femur on 15/4/09.
28.2.09
Laparoscopic salpingectomy and removal of a chronic right tubal ectopic pregnancy.
3.3.09
A nightmarish lap chole. 50M with previous history of some procedure in RUQ (?subphrenic abscess drainage or cholecystostomy?). Dense mass in Calot’s triangle. After dissecting out dense adhesions with pylorus and duodenum, neck of gall bladder ligated and transfixed. POD1 reportedly leaked bile through drain, thereafter developed a big septic abscess around the drain site, opened and debrided under anaesthesia (necrotising fascitis ); developed frank faecal fistula later and was referred to DMC Ldh.
10.3.09
my own practice, first case: RIH 63M, easy Lichtenstein.
13.3.09 and 15.3.09
Two successive ‘humping right hepatic arteries’ at lap choles, one too densely adherent to cystic duct, so the gall bladder ligated at the neck.
16.3.09
Unexpected postop course for an open prostatectomy 65M. 9th post operative day, had a grand mal seizure. CT showed a big mass (meningioma?). referred for neurosurgery.
17.3.09
Tried unsuccessfully a retroperitoneal laparoscopic ureterolithotomy 50M. Space difficult to maintain due to obesity. Converted to open ureterolithotomy, a big stone in lower ureter removed.
25.3.09
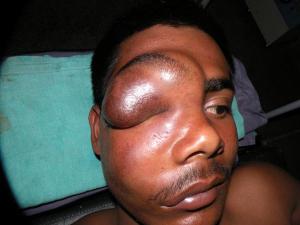
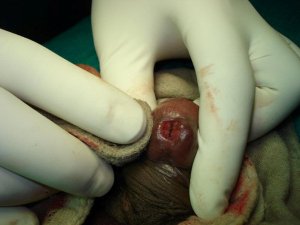
Neglected long-standing hamartoma of face 25M. Development of vision had suffered. Difficult excision of the firm and fibrotic mass almost all over the right half of the face.
26.3.09
Ill-advised and ill-fated laparotomy. 45M with h/o 4 days abdominal distension and pain. USG- collection intraperitoneal. Paracentesis – dark blood. Opened with provisional diagnosis of gangrene gut, but had actually haemoperitoneum. Nearly 2 litres of blood. Fresh bleeding coming from metastatic liver nodules, not picked up by the scan. Spurting vessels from the hard nodules near the porta, could not be controlled. Packed and referred to PGI, but died there the same day. Never had such a shocking experience earlier.
27.3.09
MS2: Occipital menigocele repaired. 1 month old female child.
28.3.09
Supposedly a thyroglossal cyst in midline 11 months old female child, turned out to be a mucous cyst only in the submandibular region (?from minor salivary glands).
A very long intersphincteric fistula-in-ano; reucurred. 50 M from Kheri, obese. All track excised. took 2 months to heal.
29.3.09
A similar high intersphincteric fistula-in-ano excised; again recurred and 50M.
30.3.09
lLaparoscopic salpingotomy for an unruptured ectopic pregnancy. Tube repaired with 4/0 vicryl.
4.4.09
Lap appy became ovarian cystectomy when the diagnosis changed to ruptured ovarian cyst on laparoscopy. 25F.
7.4.09
3 difficult cases:
Left nephrectomy for renal cell carcinoma. Obese 54 M, father of an MD psychiatry doctor from Ludhiana. A single episode of haematuria. CT showed 5 cm tumour left kidney upper pole. Anterior transperitoneal approach, the whole thing mobilised along with spleen and tail of pancreas. Spleen preserved, but some of tail of pancreas, being adherent with the tumour, excised along with the specimen. This tail was closed with silk sutures.
Lap chole 50 F, difficult due to thick-walled gall bladder, empyema and gangrene of wall of gall bladder.
Hydatid cyst of segment 8 of liver, very high under the diaphragm and adherent to it. Very difficult approach and procedure. All membranes removed after injection of hypertonic saline. Cavity obliterated with capitonage and at the end with a plug of omentum. Had fever postoperatively from POD1 and persisted for nearly a month, due to atelctasis and a patch of pneumonitis right lower lung zone.
10.4.09
Converted lap chole after finding very dense inseparable omental adhesions with gall bladder all over down to the neck, producing a big hard mass. 25 years young male with previous ERCP and ES for CBD stones, stones removed and CBD stented. At open operation, gall bladder opened, stones removed and a partial cholecystectomy done, ligating the neck from within. Finding a central dark patch ( a possible perforation of pyloroduodenal area) on the surface of the centre of the thick inflammatory mass which had been separated from the gall bladder, decided to open it and freshen it up and close it again, but when it was cut with scissors with this intent, the mucosa still escaped the scissors, so was closed with seromuscular sutures. Another new experience.
17.4.09
Bilateral inguinal direct herniae repaired with mesh. Dr Sat Pal from Mansa.
A high interphincteric fistula again. 9 cm long track on MRI. 50 M again with recurrence. The track went rght upto the ischial tuberosity. Postop had foot drop, related to the lithotomy position, recovered over 2 months.
21.4.09
A perianal abscess, extensive, going almost all around the anal opening except the left lateral 1/3rd of it. 25M who turned out to be diabetic and the abscess unexpectedly bad with extensive necrotic areas in it. All thoroughly debrided.
22.4.09
MS6: PUH repair. 62M.
23.4.09
An abdominal hysterectomy getting into unexpected problems. A simple easy and satisfactory TAH done on a 60 F. Next day reported to be in anuria with passage of scanty blood-stained urine and very low BP. ? ligated ureters, ruled out on ureteroscopy and contrast study. Explored on seeing blood oozind out of the wound and suspicion of ?intraperitoneal haemorrhage. Found none, except ooze from all over, ?DIC. Then it transpired that she had a blood transfusion yesterday just before the operation. Mismatched?
30.4.09
Excision of a left thigh swelling. Cystic hygroma. 10 year old male child. MRI suggested a hamartoma.
7.1.09
Wedge excision of cancer lip – 45 M with zarda addiction.
9.1.09
A satisfactory TEP after a long time. Right indirect inguinal hernia.
2.1.09 to 16.1.09 vacation
16.1.09
An easy appearing appendicectomy became a hemicolectomy. A fit young 30 M with presentation like appendicitis. On palpation at surgery, the appendix was found to be densely adherent with a high-lying caecum which also had a palpable mass in it, and the right colon was quite considerably shortened. A few small lymph nodes were also palpable in the mesentery. All this was excised and an ileocolic anastomosis made. Path report later was non-specific inflammation. Nonetheless, the treating physician decided to give a course of ATT.
24 and 25 jan –
Conference in Delhi on ‘complications in laparoscopic surgery’ attended. Nicely organised by delhi chapter of ASI.
1.2.08
a shocker of a news – 5 babies in phototherapy unit of rajendra hospital paediatric department burnt alive.
2.2.09
Principal of medical college (dr JPK shergill) and junior resident on duty suspended.
3.2.09
Strike by juniour doctors association against the suspension.
5.2.09
Suspensions of both the JR and principal withdrawn!.
6.2.09
Information that transfers to Amritsar are being made tommorow led to my decision to resign from service.
7.2.09
Gave my premature retirement notice to Principal’s office and resigned.
8.2.09
Gave departure report to Principal’s office.
9.2.09
Inguinal canal of a 6-year-old male child explored for undescended testis on the right, only to find that one was easily found in the canal and another one coming through the ring from inraabdominal location. Thus both testes coming from same side. Never had seen or heard of such a thing.
ASI conference at Ludhiana, urethral stone in navicular fossa and partial urethral duplication.
Posted on: January 4, 2009
27.12.08 to 30.12.08
ASI conference at Ludhiana, actually a big mela. Attended for two days 26 and 27 december. Chaired a session on 27th.
1.1.09
25 M with presumed urethral stricture. Bouginage sounded a stone in the navicular fossa. The stone simply removed with a curved haemostat and a scoop.
4.1.09
A partial urethral duplication, just a small 1 cm tunnel above the actual urethra (with a septum between the two) in the distal penile urethra at the tip. 20 M with no symptoms, but rejected from entry into military service on this account. The septum was excised with the tip of Bovie diathermy.
12.12.08
Rectovaginal fistula arising as a result of prolonged labour (home conducted delivery by dai) . Easily approached from below (vaginally) and easily repaired. Patient from some outside town.
16.12.08
In a busy lap day, had the horror of seeing the so-called safety trocar (used for the umbilical camera port entry) causing intraperitoneal bleeding, shock (sudden unrecordable BP) and a big retroperitoneal haematoma seen in front of the scope on introduction of the telescope. Immediately converted and the rent in the aorta controlled with finger pressure and then sutured with 3-0 prolene. Continued to do open cholecystectomy with the courageous anesthetist’s consent. Needed 2 units of BT immediately for resuscitation and 2 more in the ward later.
Good quick recovery afterwards, although the patient was left with a long laparotomy incision.