Author Archive
Chronic venous leg ulcer, persisting despite multiple interventions; and a breast cancer incorrectly diagnosed
Posted on: August 20, 2023
5.5.23
A 45 years old patient presented with a history of suffering for 5 years from varicose veins and a non-healing ulcer in the right lower leg. Had undergone surgery for varicose veins twice in RHP, first in 2018 and then again in 2020. A third surgery was done in a private hospital in 2023. On examination the ulcer and varicose veins were still present. Was advised a repeat venous doppler ultrasound study, and compression dressings/stockings in the meantime. He never reported back. However, the two prescriptions he carried were the following.


4.5.23
A wide local excision of a breast lump was carried out in a 45 years old female (Dr Jagga’s case), presuming the the lump to be not malignant because the FNAC had not reported carcinoma, but only atypical ductal hyperplasia. However, at operation a clear skin dimple was noted in the left upper quadrant, strongly suggesting cancer (this clinical sign was perhaps not noted by the clinician). The mammography report was BIRADS IV/V category (highly suspicious).



The biopsy report, as expected, was IDC. An MRM was done on 25.5.23.
2.5.23
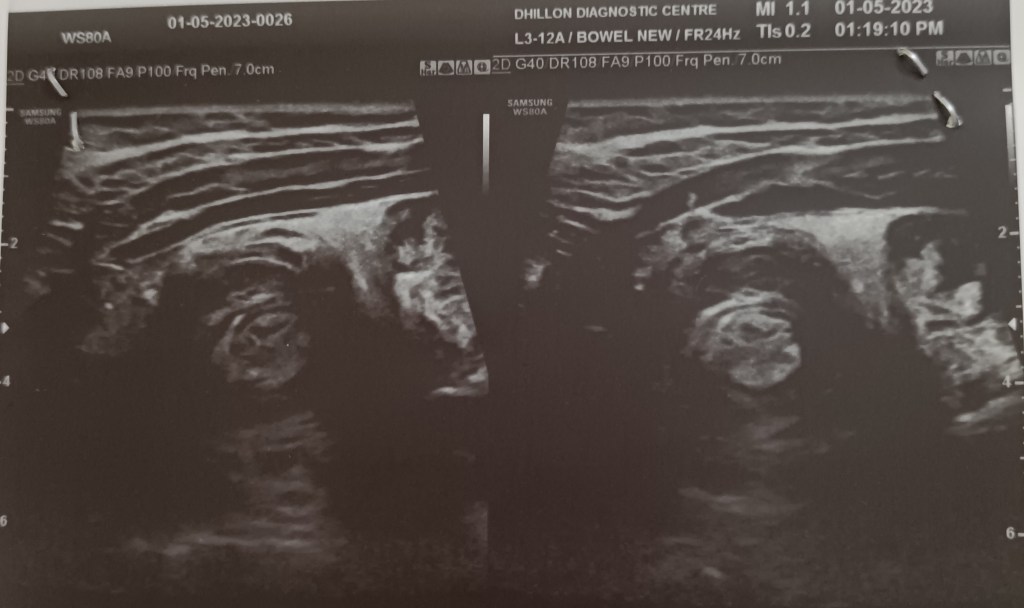
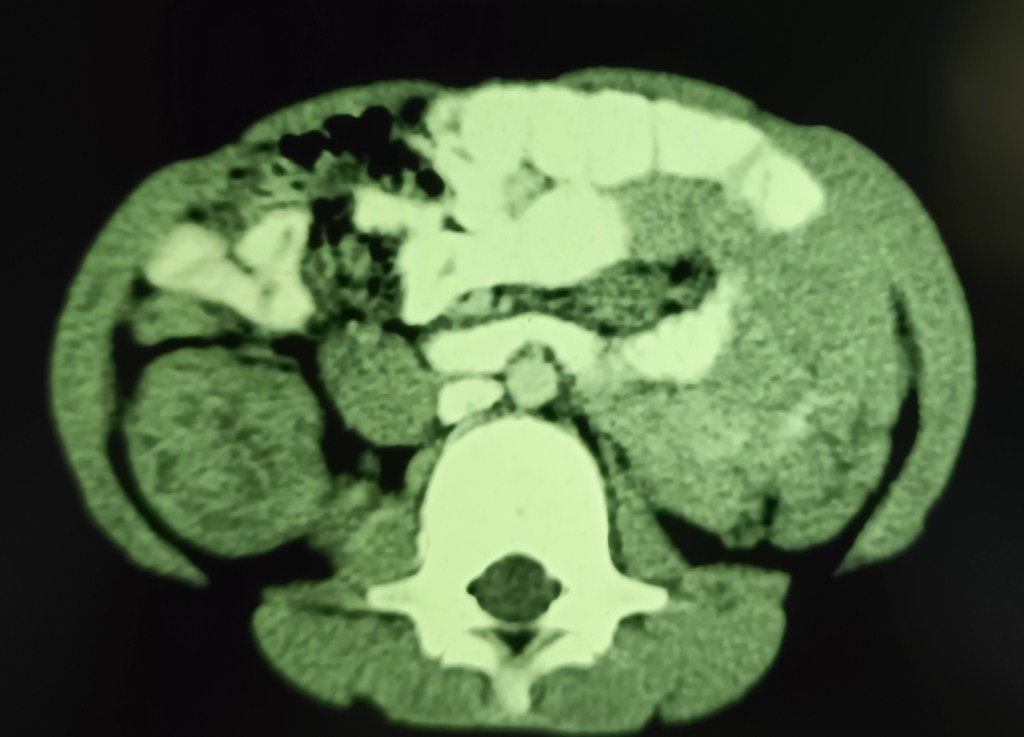
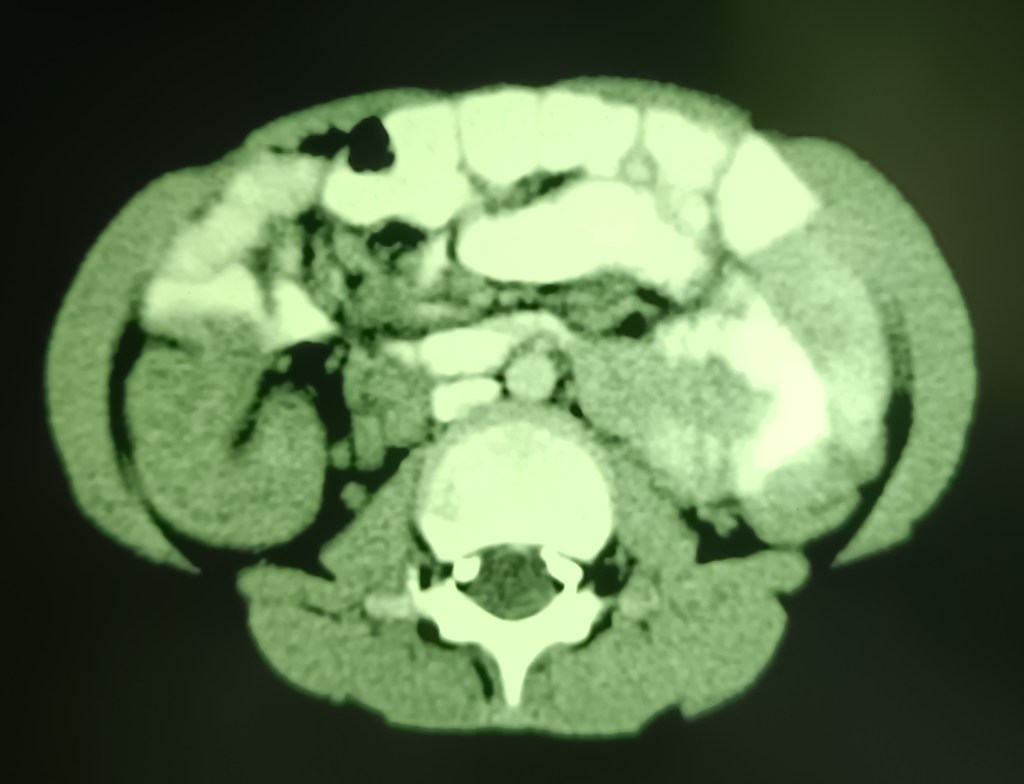
A 7 years old male child admitted with acute abdominal pain showed classic signs of target sign/doughnut sign/pseudo-kidney signs on ultrasound and a mass effect in right iliac fossa on CT. However, the child’s condition improved rapidly and in a few hours he became clinically better and pain free, suggesting spontaneous reduction of the intussusception. Recovered completely on conservative treatment and was not operated.

3.5.23
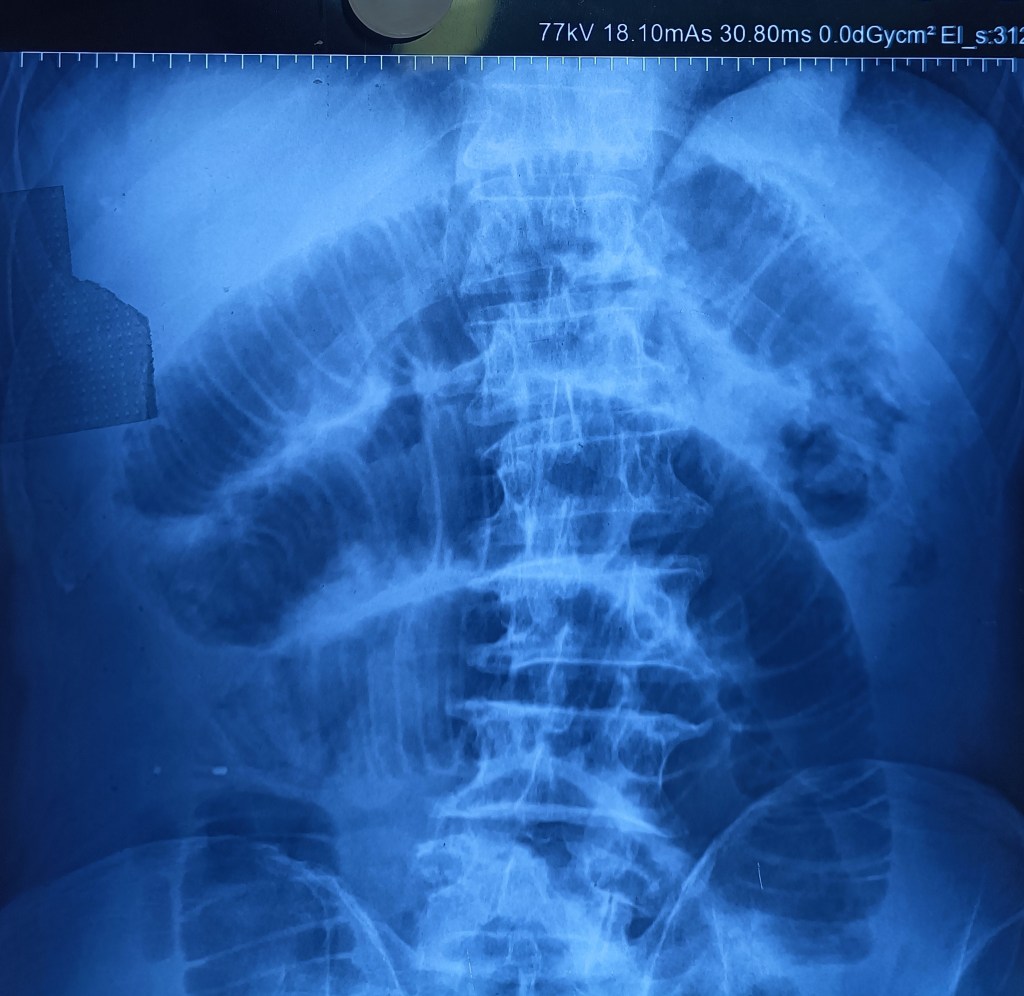
An elderly man (70 years old), a Nihang, had been having an inguinal hernia for nearly 20 years. This had now grown hugely, extending down into the scrotum, with abdominal X-ray showing signs of intestinal obstruction. However, he was adamant at not having surgery.
12.2.23
A 35 years old female (from Sunam) presented with a chronic left parotid swelling. An ultrasound scan reported a heterogenous mass in the left parotid gland, and a CT scan showed a 22×42 mm sized mass in the superficial lobe; the FNAC suggested chronic reactive lymphoid hyperplasia. At superficial parotidectomy, the superficial lobe was found to be diffusely enlarged (no discrete mass with discrete margins), and was removed. Biopsy reported reactive lymphoid hyperplasia.


Feb, 2023
An old man, nearly 70 years of age, presented in OPD with huge plexiform neurofibromatosis of the face and back, with a history going back to more than 50 years. He was now distressed particularly by the big facial lesion and wanted excision.


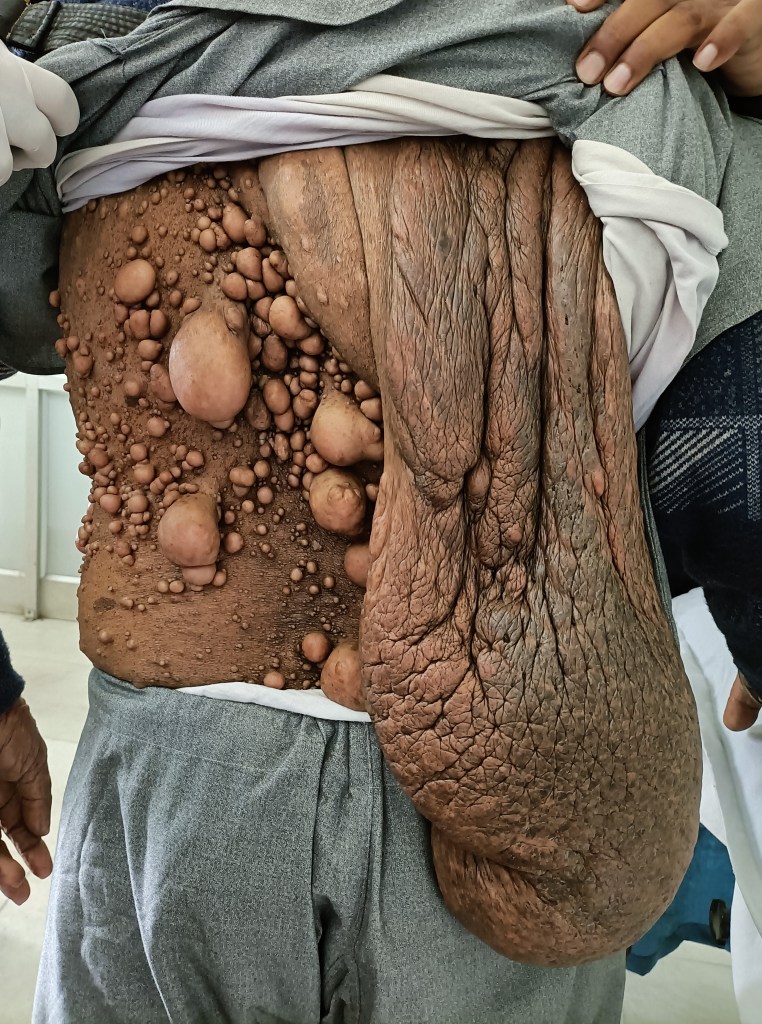
The facial lesion had brought down his pinna too, and he was unable to hear on that side. An MRI showed much deeper involvement, with destruction of the facial and cranial skeleton, suggesting malignant transformation. Was referred to neurosurgery department PGI.

Two bad experiences – messed up piles, fissure (Munchausen syndrome) and appendix cases. Examples of poor preoperative planning and preparation
Posted on: June 13, 2023
25.1.23
A 45 years old female had been posted for surgery for piles and a possible fissure too. At operation, the patient turned out to be very uncooperative, moving restlessly and talking incessantly and loudly. The anaesthetist had to use propofol to the spinal anesthesia to calm her down. An examination under anesthesia revealed no piles and no fissure, albeit a small perianal posterior skin tag was present. This was just excised. The anesthetist during the procedure had revealed her history of 4 previous surgeries for similar complaints. Munchausen syndrome was suggested as the possible diagnosis and was agreed to in the end with the treating physician.
The other case, a 45 years old male, was posted for appendicectomy. At operation, on palpation under anesthesia, a firm fixed mass was palpable. Again during surgery, the anesthetist gave the history! The patient had had pain for 4 months, was an opium addict and continued to neglect his symptoms. The incision had to be extended (RM), and a retrocecal chronic abscess and appendix were found with great difficulty. The pus was drained and the cavity washed clean after removing the appendix.
A 50 years old female was reportedly operated for cholecystectomy – an open operation, which was reportedly abandoned due to adhesions, as per the relatives’ version as there was no medical record available. However, a trial of laparoscopic approach was found to be quite easy and unremarkable. Possibly the operator was a beginner.
11.1.23
Another 50 years old lady had been having repeated scans (US and MRCP) reporting a contracted gallbladder with stones. The MRCP report also mentioned an ‘indentation’ on the main bile duct, suggesting pressure by a stone. At lap chole, the gallbladder was actually of normal size, albeit packed tightly with stones. The Calot’s dissection was difficult due to these stones, and the short cystic duct, dissected with difficulty, was ligated with no 1 vicryl.
27.12.22
A 50 years old male patient had to suffer for more than a year with different manifestations of gallstone disease:
Admitted with a local practitioner with acute pain RUQ abdomen, diagnosed as acute cholecystitis due to gallstones, largest stone being 14.5 mm. The ultrasound also reported wall thickening of the gallbladder wall, suggesting a longer history of the disease.

On 30.11.22, he was admitted again with a more severe attack of similar pain. This time, the ultrasound showed diffusedly thickened walls of the gallbladder, multiple stones and a possible collection in the fundal region, suggesting a perforation. A CT scan was suggested.
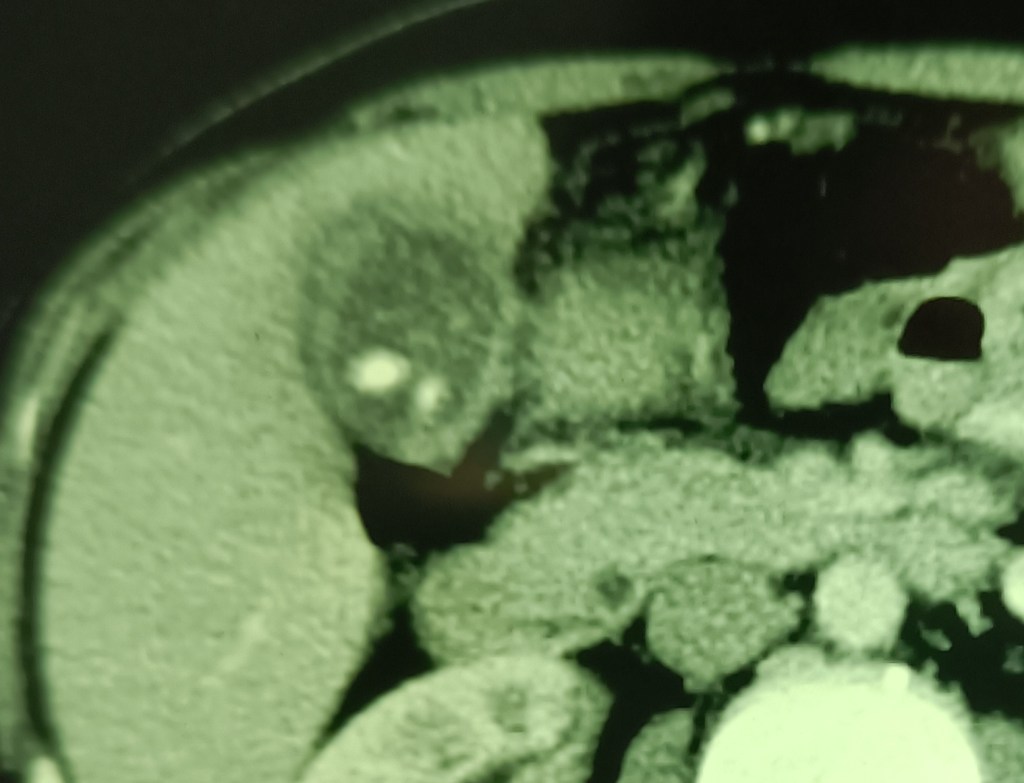
This reported distended gallbladder with diffusely thickened walls and multiple stones.
On 27.12.22 was admitted for lap chole. An US this time showed a wall echo complex in the gallbladder fossa. A routine lap chole was performed, resulting in the end of the suffering.
Neglected phimosis can lead to diagnostic confusion – posterior urethral valves vs neurogenic bladder?
Posted on: June 5, 2023
A 13 years old boy presented with acute painful retention of urine at night (it was actually an acute-on-chronic retention, as it came to light later) and since catheterization could not be done due to the tightly stenosed preputial opening, the bladder was emptied with a suprapubic needle. An ultrasound scan in the morning reported circumferential wall thickening of the urinary bladder and a V-shaped deformity of the bladder neck, suggesting a diagnosis of posterior urethral valves.
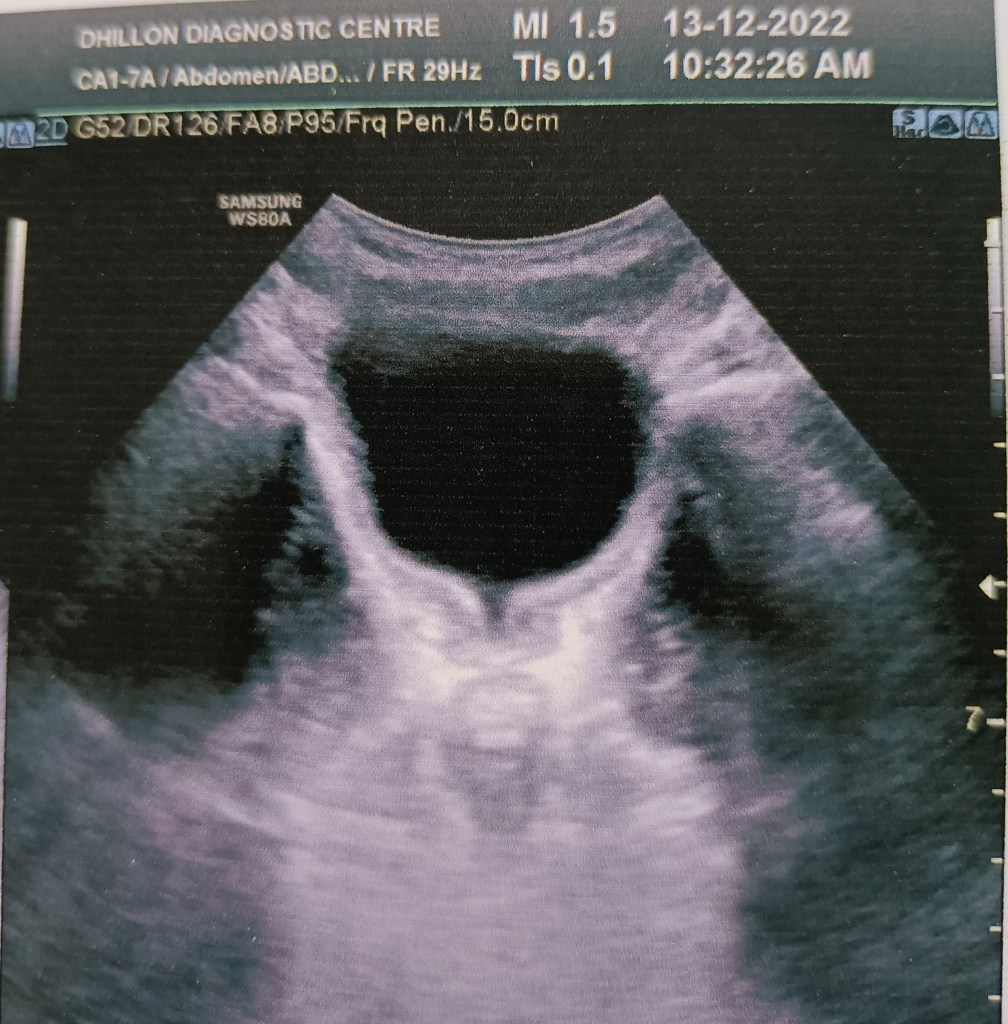

Paediatric surgical consultation was obtained and an MCU was suggested. This was done and suggested a diagnosis of neurogenic bladder while ruling out posterior urethral valves.
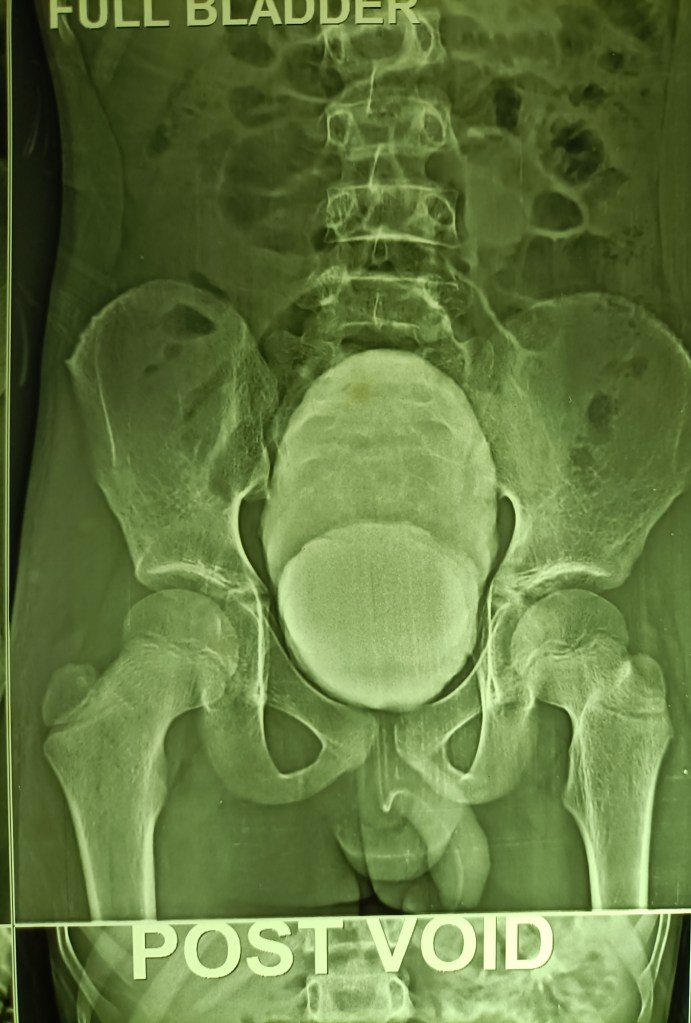
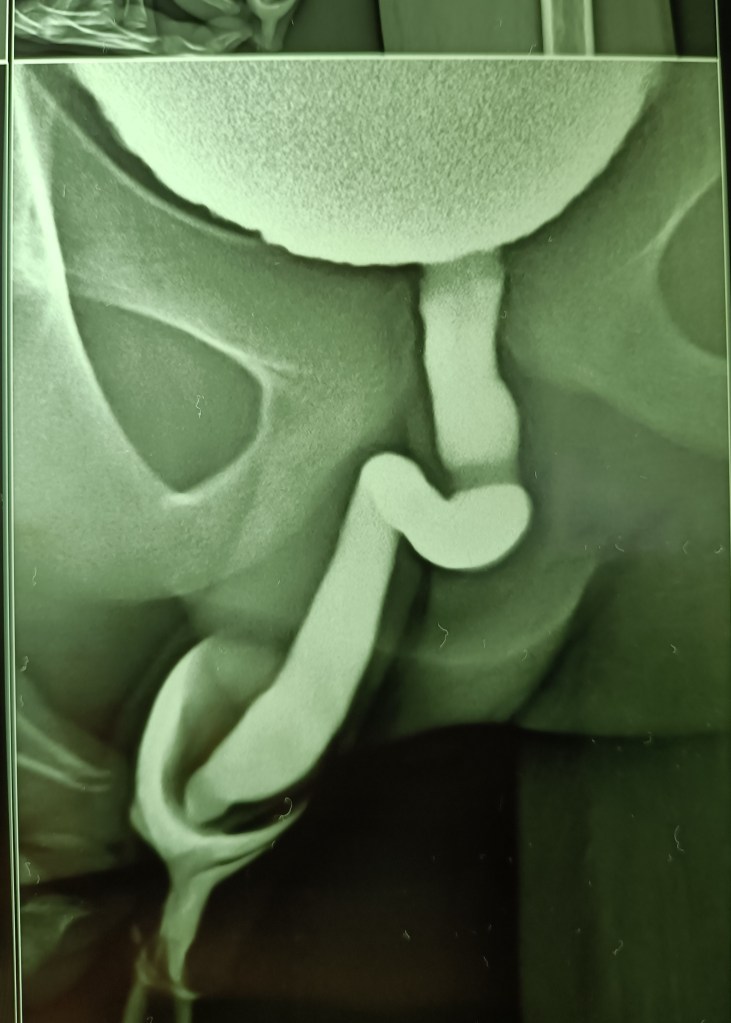
A routine circumcision was performed the same day and the child remains well thereafter.
Two lap chole lessons in one day
Posted on: June 4, 2023
19.10.22
lesson 1. Gallbladder tightly packed with small stones is better emptied of all its stone burden to make dissection easier and safer:
A 55 years old lady was admitted for lap chole after a 3 days hospitalization in some other hospital for acute pancreatitis from which she had recovered. The fact that the gallbladder was tightly packed with stones was not apparent by the look of the gallbladder, but the dissection of the cystic duct and its clipping took a long time due to small stones in it which had to be milked up repeatedly. During dissection of the gallbladder from its liver bed, its wall ruptured spilling hundreds of stones, and when all stones were removed, it was realized if we could have done that intentionally before dissection of the cystic pedicle, it would have made the procedure more safe and easy, and perhaps taking lesser time than it took otherwise.
lesson 2. A Kocher clamp with stout teeth can be very helpful in breaking big hard stones:
A lap chole in a 60 years old lady was rather easy as far as the dissection was concerned, but the single big stone (2.7 cm) caused problems in taking out the gallbladder through the epigastric port. It could not be broken into pieces with the usual ovum forceps or the bigger clawed instruments, but then the scrub nurse suggested to use the long Kocher clamp’s sharp teeth, which were eventually able to break the stone into pieces, so as to remove it without enlarging the port.